Is Meat Really Unhealthy? 6 Common Myths Debunked
In a nutshell:
- The consumption of meat has been repeatedly linked to certain diseases such as cancer or heart disease.
- However, most arguments made against meat consumption are not as strong as they are made out to be and are based on relatively weak scientific evidence.
There are not many aspects of human nutrition that attract more controversies than the question of whether we should eat meat or not.
Vegetarians and vegans remind us about the ethical aspects and the environmental impact of meat consumption.
Doctors and nutrition experts warn us about the artery-clogging properties of cholesterol and saturated fats as well as the increased risk of cancer.
Relatives remind us that we shouldn’t eat meat or we might end up with gout or diabetes.
But which – if any – of these claims are true?
This post will show you why meat is not inherently unhealthy and how it can even be healthy if combined with a low carb diet.
The content provided in this post is for informational purposes only and does not constitute medical advice. It is not intended to replace professional medical advice, diagnosis, or treatment. See further information.
1. Good studies, bad studies
So what is it?
Will meat consumption kill me or will eating a steak make me stronger and healthier?
To understand why the scientific evidence in regards to meat consumption seems to be so messy, you have to understand the difference between “good” studies and “bad” studies.
Every study has its worth and can provide a piece of the massive puzzle we’re trying to solve, but the truth is that there are huge differences in quality that can have big implications in real life.
The “gold standard” for scientific studies are randomized, controlled trials, so-called RCT’s.
In this type of study, neither researcher nor participant knows who is in the intervention group and who is in the control group.
If you’re testing a new medication, for example, the process is pretty simple: one group gets the medication, and the control group gets an identical placebo pill.
If neither researcher nor participant knows who is in the intervention group, the risk for biases is minimized and the results are much more meaningful.
As you can already imagine, it’s pretty much impossible to conduct these types of studies in the realm of nutrition.
You can’t fool anyone into thinking he’s eating a steak when in fact, he’s eating a soy protein isolate concoction.
For this reason, almost all studies about meat consumption and nutrition in general are the result of “bad” studies, that should never be used to make definitive conclusions (even though they still are all the time).
The majority of studies that concluded that meat is somehow bad for us were so-called observational studies.
This usually means that the study participants have to fill out questionnaires that contain questions on their meat consumption, for example, how much and how often they eat meat.
Now you can try to find an association between the meat consumption of the participants and their likelihood of developing a certain kind of disease – diabetes or heart disease, for example.
However, there are three major problems with these types of studies.
1.1 Correlation is not causation
First and foremost, observational studies can show one thing: a correlation.
But they can never prove causality.
Just because there’s a correlation between A and B, doesn’t mean that A causes B or the other way around.
There could be another factor C, that influences both A and B and is therefore the true cause.
A good example for this effect is the strong correlation between shark attacks and the search for the term “ice cream recipes” on Google.
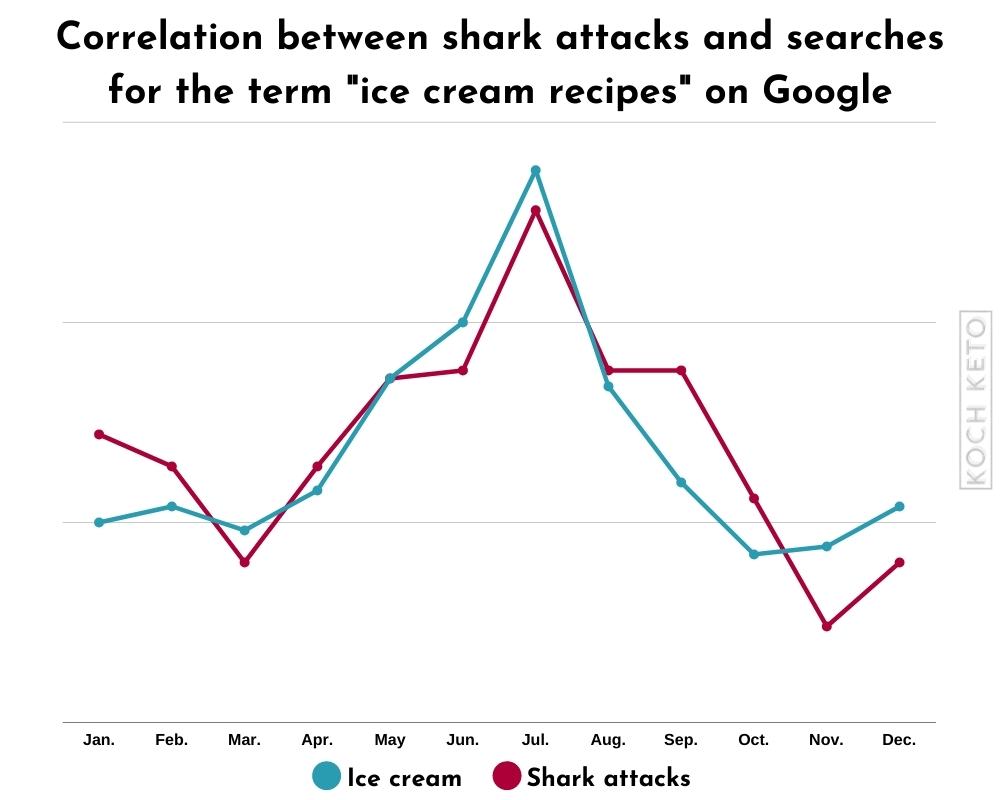
1.2 Unreliable data
The data on which observational studies base their findings is usually the result of questionnaires.
Study participants receive nutrition questionnaires and are asked to remember with great accuracy what and how much they ate during the last months or years (can you remember how many blueberries you have eaten in the last 6 months?).
This data is notoriously unreliable and does not give a clear picture of the actual eating habits of the study participants.
1.3 “Healthy User Bias”
The “healthy user bias” accounts for the fact that the average meat-eater has a much more unhealthy lifestyle in general if compared to let’s say, vegans, vegetarians, or health-focused people who have been told by their doctors to eat less meat.
We have been told for several decades (based on questionable data) that eating meat is unhealthy and we should stop doing so.
Someone who still eats large amounts of meat in 2020 probably doesn’t follow a lot of other advice he has been given by his doctor or other authorities.
It’s likely that this person who doesn’t care about his doctors’ opinion does a ton of other things that are considered unhealthy.
It is true that study participants who eat a lot of meat get sick more often, but they also smoke more, drink more alcohol, engage in less physical activity and are more likely to be overweight or obese.
Summary:
- Most studies that are done within the field of nutrition are so-called observational studies, that have major problems associated with them.
- The shortcomings of observational studies can result in distored results that aren’t truly applicable to real life.
2. Meat causes heart disease?
High quality studies failed to confirm this assumption
The same is true for cholesterol.
In contrast to conventional “healthy” diets, low carb diets tend to be higher in meat and saturated fats and still, they have a positive influence on the most relevant risk factors for heart disease.
Considering the mountain of evidence that has failed to support the saturated fat-cholesterol-heart disease hypothesis it’s probably fair to say that it’s unlikely the saturated fat or cholesterol from the meat will give you heart disease.
Summary:
- High quality studies do not support the hypothesis that the cholesterol or saturated fats from meat cause heart disease.
3. Meat causes cancer?
Especially red meat and processed meat are supposed to be cancer-causing – fish and poultry get a much better rep.
The World Health Organization (WHO) has even put processed meat into the same category as cigarettes!
Consuming processed meat increases the risk of developing colon cancer by 18%.
There doesn’t seem to be much room for debate, right?
Association between meat and cancer is based on observational studies
First and foremost: they can only show a correlation, but never causation.
Yes, meat consumption and bowel cancer are correlated, but this doesn’t prove that meat causes bowel cancer.
Like mentioned in the first section, one of the biggest problems with observational studies regarding meat consumption is the “healthy user bias”, meaning that the average meat-eater is generally not as healthy as someone who deliberately limits his meat consumption (and does tons of other things that he deems to be good for his health).
The average meat-eater does tons of other things that can increase his risk for cancer, like smoking or being overweight/obese.
Being overweight/obese is in fact, an even bigger risk factor for developing bowel cancer than smoking.
Granted, most researchers try their best to account for all of these factors, but nobody can garantuee that the final conclusion is completely free of distrortions and biases.
Is eating meat truly as bad as smoking?
But there’s a difference between the association between lung cancer and smoking and bowel cancer and meat consumption.
Smoking increases your risk of getting lung cancer 20-fold.
The increase in relative risk is about 1900%.
An extremely strong association, that makes it unlikely that another factor could be responsible for the increase in risk.
In comparison: the consumption of processed meat increases your risk of getting bowel cancer 1.18-fold, or 18%.
It is therefore completely misleading to say that meat consumption is just as dangerous as smoking.
What “good” studies say
In both studies, the intervention group reduced their red meat intake significantly while the control group ate as much red meat as before.
If red meat does indeed cause cancer, we should have seen more cancer cases in the control group and fewer cancer cases in the intervention group.
But this was not the case.
The reduction in red meat consumption in the intervention group had no effect on the cancer rate.
Summary:
- Although there is a (weak) association between the consumption of red/processed meat and cancer, this does not automatically mean that meat causes cancer.
- The association between meat consumption and cancer is distorted by the fact that the average meat-eater generally lives an unhealthier lifestyle and thus has a higher exposure to other potentially cancer-causing factors.
- Two big controlled studies did not replicate the link between red/processed meat consumption and cancer.
4. Meat damages the kidneys?
Damaged kidneys don’t function as well as healthy kidneys and a higher protein load could lead to additional stress being placed on them which might result in a worsening of the disease.
But most people don’t have chronic kidney disease – what about them?
There is no evidence whatsoever that protein damages healthy kidneys.
Even amounts that are almost impossible to reach with a normal diet (3g per kg of body weight or about 1.5g per lbs) had no adverse effects on kidney function.
Summary:
- People who have a chronic kidney disease should avoid consuming too much protein.
- There is no scientific evidence that too much (animal) protein damages healthy kidneys.
5. Meat makes our body “acidic”?
Usually, animal products leave behind acidic ash while most plant-based products leave behind alkaline ash.
Followers of the “alkaline diet” promote the idea that humans should avoid acid-producing foods and stick to alkaline foods.
This is supposed to have a beneficial impact on our health, especially in regards to our bones.
While it is true that eating specific foods can influence the pH level of our urine for a short amount of time, it is not true that we can change the pH level of our blood and thus the rest of our body.
The pH level of our blood is tightly regulated by our body and remains constant at about 7.4.
Furthermore, clinical studies do not support the acid/alkaline theory in regards to our bone health.
Summary:
- The food we eat does not influence the pH level in our blood.
- Clinical studies did not confirm the acid/alkaline theory in regards to our bone health.
6. Meat causes gout?
Some women who have experienced a gout attack describe the pain as being worse than that of childbirth!
So it seems fair to say that gout can be an extremely debilitating disease you want to avoid at all costs.
A meat-heavy diet is often stated as the cause of gout, but as you will see, this is not correct.
The origins of gout
Normally, we simply excrete the uric acid without problems and never experience a gout attack.
In the vast majority of gout patients, however, this excretion process does not work properly.
The kidneys of gout patients are not able to properly clear the uric acid from the body which consequently leads to an increase of the uric acid levels in the blood and finally, if the uric acid load gets too high, to a gout attack.
Does a diet high in animal protein cause gout?
At the same time, however, the excretion of uric acid increases as well and the level of uric acid in the blood will remain constant or may even decrease.
Even though meat consumption is often linked to gout in observational studies, a diet high in (animal) protein has no negative effect on uric acid excretion and may even improve it.
So the million-dollar question doesn’t seem to be what causes a temporary increase in uric acid levels, but what causes the diminished excretion of the uric acid through the kidneys.
The true causes of gout
1. High insulin levels & insulin resistance
A chronically high level of insulin leads to diminished excretion of uric acid through the kidneys.
Type 2 diabetes (which is basically end stage insulin resistance) is actually the number one cause of preventable kidney failure.
But that’s not all, even in healthy people insulin will lead to poorer excretion of uric acid through the kidneys.
2. Fructose
Even though fructose is often seen as harmless “fruit sugar”, it can play a major role in the development of gout.
That’s because the overconsumption of fructose can lead to insulin resistance of the liver which in turn can result in the development of a non-alcoholic fatty liver and type 2 diabetes.
In addition, high fructose intake leads to an increased uric acid level in the blood.
3. Alcohol
Alcohol inhibits uric acid excretion and can thus contribute to the development of gout.
Meat is not the cause of gout
Yes, meat can worsen symptoms of gout if you already have it, but there’s no evidence (besides weak associations in observational studies) that meat is the cause of gout.
If you pair insulin resistance, overconsumption of fructose, and overconsumption of alcohol with high consumption of meat (which, incidentally, sounds just like something the average meat-eater does), you may end up with a gout attack.
But meat wasn’t the starting point – poorly functioning kidneys were.
Summary:
- Gout is caused by the diminished excretion of uric acid from the body, which can lead to the accumulation of uric acid crystals in the joints.
This, in turn, can cause a gout attack with symptoms like severe pain and swelling. - High insulin levels, insulin resistance, overconsumption of fructose, and overconsumption of alcohol are the true cause of the diminished excretion of uric acid through the kidneys.
There’s no evidence that the consumption of animal protein leads to poorer uric acid excretion. - Meat consumption can worsen the symptoms of gout if there are already existing problems with uric acid excretion, but meat is not the cause of gout.
7. Meat causes diabetes?
That meat allegedly causes type 2 diabetes is a prime example of the unreliability of observational studies.
Like with many other diseases, observational studies have found an association between meat consumption and type 2 diabetes.
However, the same shortcomings that were mentioned before apply here as well.
The average meat-eater drinks more alcohol, smokes more, carries more weight and eats an unhealthier diet in general.
No wonder then, that these guys have a higher rate of type 2 diabetes than, let’s say, crossfit-crazy vegetarians.
However, there are many other reasons why it is very unlikely that meat consumption causes diabetes.
Type 2 diabetes is basically end-stage insulin resistance
Diabetes type 2 is more or less the “final form” of insulin resistance.
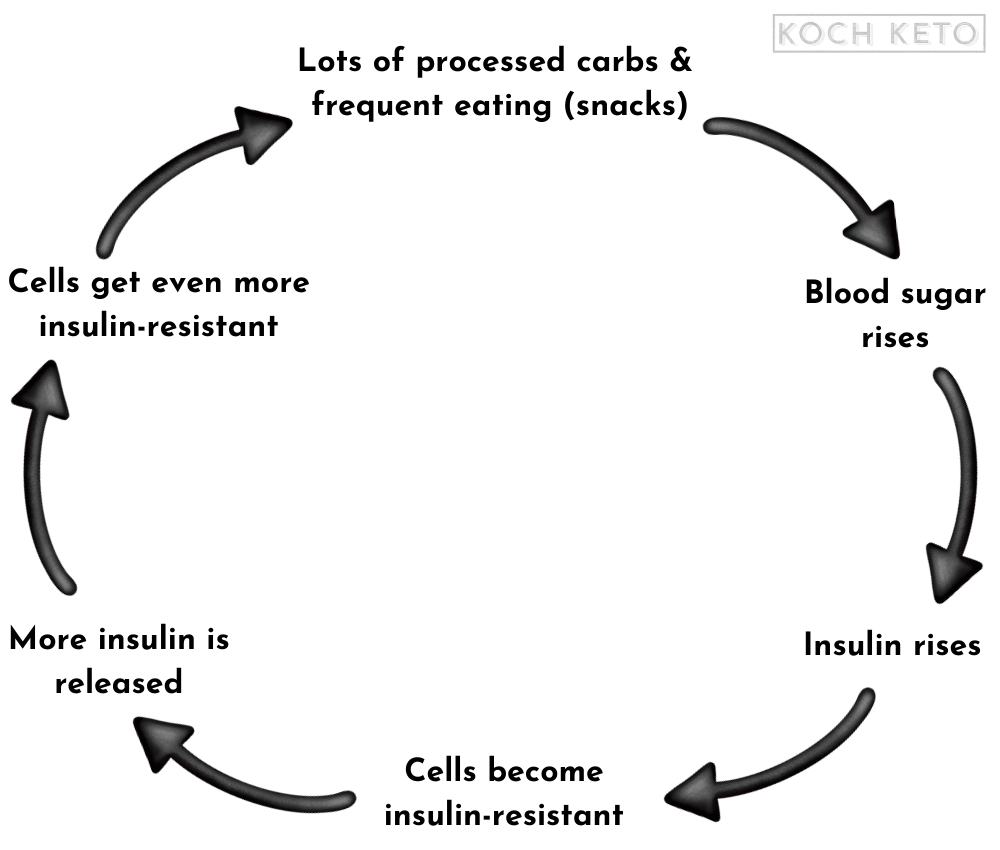
Insulin resistance develops when the body is exposed to large amounts of insulin for too long and too often.
After a while, our cells start to ignore the signals of insulin and become insulin-resistant.
But our body needs to get the energy in the form of sugar out of the bloodstream and into the cells to survive, so it reacts by releasing even more insulin.
But this in turn leads to our cells becoming even more insulin-resistant.
When the body isn’t able anymore to clear its bloodstream from sugar, it will rise steadily until it reaches a point where it starts to wreak hammock.
At some point, this vicious cycle will most likely end in the diagnosis of “type 2 diabetes”.
Meat consists mainly of fat and protein and even though fat and especially protein do also increase insulin levels, the amounts are not comparable to the significantly more likely causes of insulin resistance:
Sugar and processed carbs.
The overconsumption of sugar can lead to insulin resistance of the liver, which in turn can result in the development of a non-alcoholic fatty liver & type 2 diabetes.
In combination with the flood of highly processed carbs that cause our insulin to spike tremendously every time we consume them, they are much more plausible candidates for the development of insulin resistance than meat is.

Low carb and keto diets improve type 2 diabetes
If meat does indeed causes type 2 diabetes we should, therefore, see more diabetes cases or a worsening of the disease in people who follow a low carb diet.
However, the exact opposite is what happens.
Dozens of controlled studies show an improvement of type 2 diabetes by following a low carb diet, while taking less medication!
Summary:
- Meat is not a very likely cause for the development of insulin resistance/type 2 diabetes as it doesn’t release much insulin and it conflicts with the success of meat-heavy low carb diets in improving type 2 diabetes.
- The true causes of insulin resistance are most likely: too much sugar, too many processed carbohydrates and too many meals (mostly in the form of high carb snacks).
8. Health benefits of meat
We are constantly bombarded with negative headlines and never get to hear about the positive aspects of meat consumption.
From this perspective, eating meat is solely something humans like to do, but shouldn’t do.
But it is not true that the question of whether humans should eat meat or not is simply a question of pleasure vs health.
Contrary to popular belief, meat is not just a tasty slab of protein – no, meat is one of the most nutritious foods on our planet.
And not only that, there are also a number of nutrients that are either exclusively found in animal products or are much better absorbed from animal sources than from plant sources.

Nutrients in meat, fish & eggs
- Vitamin D: Fatty fish and cod liver oil are the only noteworthy dietary sources of vitamin D.
Plants do not contain bioavailable vitamin D. - DHA: DHA is an essential omega-3 fatty acid and is primarily found in fatty fish.Plants typically don’t contain DHA, but a different omega-3 fatty acid (ALA), which is poorly converted by the human body into a bioavailable form (less than 5%).
- Iron: The human body absorbs about 3-14 times more iron from red meat (heme iron) than iron from plant sources (non-heme iron).
- Zinc: Zinc is mostly found in animal products. Zinc from plant sources is usually less well absorbed by the body.
- Vitamin B12: Bioavailable vitamin B12 is exclusively found in animal products.Vitamin B12 found in plants is not biologically active and cannot be utilized by our body.
- Vitamin K2: Vitamin K1 and K2 seem to play completely distinct roles in our body, which is why some experts have suggested that they should be considered two separate nutrients.
While vitamin K1 is primarily involved in the process of blood clotting, there is much evidence to suggest that vitamin K2 contributes primarily to our bone and heart health. Vitamin K1 is mainly found in leafy green vegetables, whereas vitamin K2 is mainly found in animal products. - Vitamin A: Contraty to popular belief, carrots and other plant sources don’t actually contain vitamin A, but ß-carotene, a precursor for vitamin A. Only about 5-7% of ß-carotene is converted to vitamin A.
However, some individuals are even worse at carrying out this conversion due to genetic predispositions.
Summary:
- Meat, fish and eggs are very nutrient-dense.
- Some vitamins and minerals are exclusively found in animal products or can be much better absorbed from animal sources than from plant sources.
9. The bottom line
Although meat has been part of our human diet for about 2.5 million years , only in the last 100 years it has allegedly lead to the disastrous health consequences we see today.
The diets of several indigenous populations like the Masaai and Samburu from Africa , the Inuit from the Canadian Arctic , the Chukchi from Russia or the Brazilian gauchos are based entirely or primarily on animal products and yet these tribes are virtually free from the diseases that are attributed to meat consumption in our world.
Weak associations are used as definitive proof for the harmful effects of meat consumption and yet, high-quality science usually fails to replicate those findings.
A closer look at the body of evidence against meat consumption reveals:
Then what’s making us sick?
Meat is the bogeyman of our society.
Instead of concentrating on the actual cause of so many diseases, we keep our eyes locked on our meat consumption and try to turn weak associations into rock-solid science.
Nobody sees the elephant in the room:
insulin resistance.
Insulin resistance is at the root of dozens of diseases such as type 2 diabetes, Alzheimer’s, cancer and heart disease.
Interestingly, many of the diseases that are likely caused by insulin resistance are continuously blamed on our meat consumption.
Meat is more than pleasure
It is not true that the question of whether we should eat meat or not is only a matter of pleasure vs health.
Animal products contain nutrients that we cannot get from any other source and these nutrients are important for a healthy body and mind.
Low carb and keto diets usually contain more animal products than other diets and we hope that this article was able to ease your mind and show you why that doesn’t automatically mean you will soon die of a heart attack or cancer.
The opposite is likely true, as low carb diets are very effective against the most probable cause of most modern diseases – insulin resistance.
FAQ’s
Is meat healthy or unhealthy?
Some nutrients are found exclusively in animal products or are more readily absorbed from animal products than from plant sources.
What are considered red meats?
- Pork
- Beef
- Mutton
- Game
- Lamb
- Veal
Does red meat cause cancer?
For example, the average meat-eater smokes more, weighs more, drinks more alcohol, and follows a much more unhealthy lifestyle in general than someone who is consciously paying attention to what he eats (i.e. vegetarians or vegans).
Which kind of meat is the healthiest?
Fattier cuts of meat usually also contain more nutrients than lean meats.
However, organs such as liver are by far the most nutrient-dense.